Special delivery: Mayo Clinic’s technology helped with birth during snowstorm
Published 7:15 am Tuesday, February 12, 2019

- Dayoni Hash holds her daughter Nevaeh, who decided to pick the coldest day of the year to enter the world. Photo provided
While a winter storm was raging outside on what was considered to be one of the coldest days in Minnesota history, Dayoni Hash of Blooming Prairie was fighting a storm of her own — going into labor.
Her water had just broken, though she was seven weeks early from the due date. Weather conditions were rapidly deteriorating outside and an advisory was issued for the impending storm, meaning no ambulances were able to get to her house.
Yet, the Austin native had to make the decision, along with her boyfriend Roger Loth, to make the drive to Mayo Clinic Health System in Austin to deliver their baby girl safely and to get the proper medical attention needed for the newborn.
“The vehicle almost didn’t start,” Hash recalled of the night. “There wouldn’t have been ambulances that could’ve come to get us because of the weather. It would’ve been way worse.”
Mayo Clinic Health System-Austin was prepared to receive Hash and her baby on that cold night. The hospital was short-staffed because of the weather conditions, but they were ready to give the best care they could to help with the emergency delivery.

Dayoni Hash holds her daughter Nevaeh, who decided to pick the coldest day of the year to enter the world. Photo provided
When the couple rushed to the hospital, caregivers assessed that Hash was already dilated to six centimeters, unbeknownst to her. Within 45 minutes, she reached eight centimeters. The baby was also in breech, prompting an emergency Caesarean section. They needed to act fast to give critical care to the newborn in the precious hours after birth with assistance from an neontatologist, who is normally based in Rochester.
So, they decided to use teleneonatology. Neonatologists are pediatricians who specialize in medical care of newborns, especially ones who are premature or sick. Mayo Clinic’s Teleneonatology Program assists with bringing a neonatologist’s expertise to the bedside of any newborn who needs critical care, regardless of where they are born, via a private and secure audio-video connection.
“The situation was unique since transfer on ground and air was not available,” said Brena Loucks, one of the nurses who assisted with Hash’s birth. “We needed extra eyes and guidance until the transfer team got here, and we have used telenenatology quite a few times.”
Nicole Meyer, also a nurse who assisted with the birth, shared her sentiments about the delivery.
“We weren’t able to transfer the baby for nine hours,” Meyer said, “and we needed to use the technology for a lot longer.”
Dr. Robert Johnson of the Department of Pediatrics in the division of neonatology, who is based in Rochester, personally assisted with the birth. However, it was in a way that Hash didn’t expect.
“I heard the doctor, but I personally didn’t see him,” she said. “I heard him the whole time, and they got the baby out. I thought he was in the room and when the nurses said they were all going to the nursery, I was expecting him to be here in person. When I saw him roll past the screen, I was like ‘oh, OK.’ I didn’t even know technology like that existed.”

RNs Nicole Meyer, left, and Brenda Loucks are photographed with Dr. Jennifer Fang, live from Mayo Clinic Hospital in Rochester. The nurses were part of an amazing birth during the year’s harshest conditions when the polar vortex swept down, taking part in a c-section as Dr. Richard Johnson watched over the InTouch Health device remotely.
Eric Johnson/photodesk@austindailyherald.com
A will and a way
Johnson shared how difficult the circumstances were with the treacherous weather conditions on the night that Nevaeh was born and what decisions went behind the night of her birth. With newborns who need the neonatal unit in Rochester, teleneonatology proves itself to be a lifeline.
“It started off as a typical call, and I was told that a premature baby needs our help,” Johnson said. “We were making calls about transportation arrangements given severe weather with blowing snow. Then, we were told weather would not permit a helicopter flight … the weather was so bad they called snow plows off the roads. We felt it was not safe to send an ambulance that might get caught in a drift or slip into a ditch, and that would be difficult to rescue the ambulance team. I was told they would not be able to send the ambulance out until conditions improved.”
During those hours, the vital assistance that teleneonatology provided to the staff at the Austin site proved to be a textbook example of why it was needed in a situation where a few hours could have changed the outcome.
“The ideal situation would be if there’s enough time, the mom would be transported to Rochester Methodist Hospital,” Johnson said. “That’s not always possible. Sometimes, a hospital like Austin’s has to do the initial care for a baby until our transport team can come.”
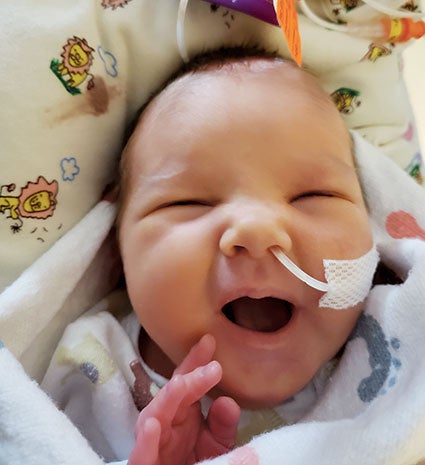
Nevaeh Rose Loth chose a difficult night for her birth, entering the world where temperatures were reaching close to 60 below with windchill and when Mayo Clinic Health System in Austin was short-staffed. Photo provided
Initially when Mayo Clinic rolled out the teleneonatology system in the past, there were several enhancements made to improve the quality of services and care that doctors could make to community hospitals around the area. Mayo established this system through 11 hospitals in the region. The somewhat new technology prevents doctors from having to leave the procedure for assistance, instead allowing them to have someone on the screen ready to step in with their expertise.
“It started with an iPad, and now it’s its own machine,” said Crystal Studer, nurse manager of women’s special care unit at Mayo Clinic Health System-Austin. “You can control the view of what’s on the screen and make a phone call on the machine, and listen to the heart and lungs and the connection is crystal clear. It really has come a long way.”
With Austin’s campus not doing these types of procedures frequently, it was important that a neonatologist would be available to assist with guiding staff at a branch campus. Having Johnson being able to use teleneonatology, especially given the storm, was a godsend.
“It was crucial to have a neonatologist visualize and walk our RNP (registered nurse practitioner) through this,” Studer said. “It was important that he was giving her feedback while doing this and being there in an instant.”
Specifically with Hash, Johnson, who has been in practice with newborns since 1987, was able to use the teleneonatology program to immediately advise the care team in Austin using a real-time audio-video telemedicine connection. During his time using the technology, Johnson said the advancement in providing care to patients has vastly improved, including care for those who live in rural communities where severe weather could be detrimental to their access.
For three hours, he stayed on the line with the Austin team to ensure that Nevaeh’s aftercare would be successful while transport teams prepared to get her.
“Given our challenges of weather and geography, telemedicine has been a tremendous help,” he said. “We actually gave presentations to use this equipment in Norway last fall, and there’s been really an interest in using technology like this to help in winter weather, and for hospitals far from the main center … we’re really thrilled on how things worked out with this and with all the help from the Austin staff. They have a lot to be proud of.”

Roger Loth holds his daughter Nevaeh in Rochester.
During her experience of giving birth, Hash said the teleneonatology system that allowed Johnson to be right there in the room with the medical team at Austin along with her gave her peace of mind.
“The staff was doing fine, but they did better with (Johnson),” Hash said. “They thought she (Nevaeh) would be worse off than she was, and put her on oxygen right away … him being there to help along with that really helped Nevaeh. It was definitely magic. I’ve never seen anything like that before, he was there, but not there, and he was able to help them. I was thinking, how does that work? Technology is getting better and better.”
It was 12:22 a.m. on Jan. 30 when little Nevaeh was born, weighing five pounds and 15 ounces and measuring 16 inches long. Hash and Nevaeh were both doing well after their ordeal. Nevaeh was transported first to Mayo Clinic Hospital-Saint Marys Campus-Rochester at around 8 a.m. after the storm passed, and then Hash joined her shortly after, around mid-morning.
“This did go really smoothly, considering the circumstances, it was a great outcome,” Meyer said. “Baby has been doing well. We train for these situations, and teleneonatology definitely gave me a lot of comfort, and Dr. Johnson was a great leader and offered a lot of guidance.”
Thanks to the staff at Mayo Clinic and the teleneonatology program that helped with the aftercare of the delivery, this whole experience is one that Hash plans to tell her daughter when she’s old enough.
“The care was amazing and they were absolutely phenomenal,” Hash said. “Even after I got shipped over to Rochester, the nurses there were amazing, and the care team was amazing all the way around. It would’ve been way worse, and I’m just glad everything worked out. I don’t know what we would’ve done.”




